Understanding Peri-Implantitis and its Treatment
Understanding Peri-Implantitis and its Treatment Definition and Prevalence of Peri-Implant Diseases:
Peri-implant diseases refer to inflammatory conditions that affect the tissues surrounding dental implants. Among these conditions, peri-implantitis stands out as a significant concern. It is characterized by inflammation and bone loss around dental implants, potentially leading to implant failure if left untreated.
The prevalence of peri-implantitis has gained attention in recent years, with studies suggesting that it affects many individuals with dental implants. Research indicates that approximately 20% of patients with dental implants may develop peri-implantitis at some point. This highlights the importance of understanding this condition and taking proactive measures to prevent and manage it effectively.
Differentiating between Peri-Implantitis and Peri-Implant Mucositis:
While peri-implantitis and peri-implant mucositis share similarities, it is crucial to distinguish between the two conditions. Peri-implant mucositis refers to inflammation limited to the soft tissues surrounding dental implants. It is considered a precursor to peri-implantitis, making early detection and intervention vital.
Peri-implantitis, on the other hand, involves inflammation of the soft tissues and significant bone loss around the implant. It is a more advanced and severe stage of peri-implant disease. Proper diagnosis and prompt treatment are essential to prevent further progression and potential implant failure.
Practical Treatment Strategies for Peri-Implantitis:
Managing peri-implantitis requires a comprehensive approach, focusing on controlling the infection, halting bone loss, and preserving the implant’s stability. Let’s explore some treatment options that can aid in combating peri-implantitis:
Non-Surgical Methods: Non-surgical treatments thoroughly clean the affected area and remove bacterial biofilm and calculus deposits. This can be achieved through scaling and root planning, meticulous oral hygiene practices, and regular maintenance visits.
Surgical Intervention: In more advanced cases, surgical intervention may be necessary. Procedures such as flap surgery, bone grafting, and guided tissue regeneration can help regenerate lost bone and restore the surrounding tissues’ health.
Laser-Assisted Procedures: Laser therapy has shown promising results in treating peri-implantitis. It offers several benefits, including reduced discomfort, enhanced healing, and selective removal of diseased tissues while preserving healthy ones.
Prevention and Maintenance:
Preventing peri-implantitis is always preferable to dealing with its consequences. Here are some preventive measures to consider:
Thorough Oral Hygiene: Proper oral hygiene practices, including regular brushing, flossing, and antibacterial mouthwashes, are essential for maintaining a healthy oral environment.
Regular Dental Check-ups: Routine dental visits allow for early detection of any signs of peri-implant diseases. Timely intervention can help prevent further complications and preserve the longevity of dental implants.
Patient Education: Educating patients about the importance of maintaining good oral hygiene, adhering to post-implant care instructions, and recognizing the signs of peri-implant diseases empowers them to take proactive measures and seek professional help promptly.
Understanding Peri-Implantitis
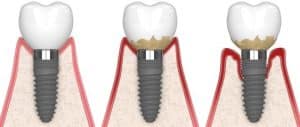
Peri-implantitis is an inflammatory condition that affects the tissues surrounding dental implants. It is characterized by the inflammation and progressive destruction of the bone and soft tissues surrounding the implant, which can ultimately lead to implant failure if left untreated.
Causes and Risk Factors of Peri-Implantitis:
Several factors contribute to the development of peri-implantitis. Understanding these causes and risk factors can help us take preventive measures and address the condition promptly. Here are some key factors:
Poor Oral Hygiene: Inadequate oral hygiene practices can accumulate bacterial biofilm and calculus around the implant site, triggering inflammation and infection.

Smoking: Tobacco use, mainly smoking, has been identified as a significant risk factor for peri-implantitis. Smoking compromises the body’s immune response and impairs blood flow, making it harder for the tissues to heal.

Pre-existing Periodontal Disease: Individuals with a history of periodontitis, characterized by gum inflammation and tooth support structure damage, are more prone to developing peri-implantitis. The bacteria involved in periodontitis can colonize around dental implants and contribute to peri-implantitis.
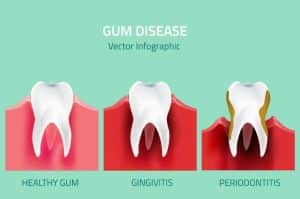
Genetic Predisposition: Some individuals may have a genetic predisposition to inflammatory responses, making them more susceptible to peri-implantitis.
Differentiating Peri-Implantitis from Periodontitis:
While peri-implantitis and periodontitis share similarities, it is crucial to distinguish between the two conditions. Here are some key differences:
Location: Peri-implantitis occurs specifically around dental implants, while periodontitis affects the natural teeth and their supporting structures.
Tissue Composition: Peri-implantitis involves the inflammation and destruction of the soft tissues and bone surrounding the implant. In contrast, periodontitis primarily affects the gum tissues, periodontal ligaments, and alveolar bone supporting the natural teeth.
Treatment Approach: The treatment strategies for peri-implantitis and periodontitis differ. Peri-implantitis may require non-surgical or surgical interventions, depending on the severity. Periodontitis often involves scaling, root planning, and other periodontal therapies to remove bacteria and restore gum health.
Symptoms and Diagnosis of Peri-Implantitis
Recognizing the Signs of Peri-Implantitis:
Timely recognizing the signs and symptoms of peri-implantitis is crucial for preventing further complications and preserving the longevity of dental implants. Here are some common signs to watch out for.
Bleeding and Inflammation: One of the primary indicators of peri-implantitis is bleeding and inflammation around the implant site. This can occur during brushing, flossing, or even spontaneously.
Increased Pocket Depth: Pocket depth refers to the space between the gum tissue and the implant. In peri-implantitis, there is often an increase in pocket depth, indicating the presence of inflammation and potential bone loss.
Suppuration and Pus: In advanced stages, peri-implantitis may manifest as suppuration or pus around the implant area. This is a clear indication of an active infection and requires immediate attention.
Gum Recession: A recession of the gum tissue around the implant can expose the implant surface and create an esthetic concern. It may also contribute to increased plaque accumulation and further inflammation.
Overview of Peri-Implant Mucositis Symptoms:
Peri-implant mucositis is a precursor to peri-implantitis, and recognizing its symptoms is essential for early intervention. The symptoms of peri-implant mucositis include:
Redness and Swelling: Similar to peri-implantitis, peri-implant mucositis is characterized by redness and swelling of the gum tissue surrounding the implant.
Bleeding on Probing: During dental examinations, bleeding upon gentle probing around the implant site may indicate the presence of peri-implant mucositis.
No Radiographic Bone Loss: Unlike peri-implantitis, peri-implant mucositis does not involve bone loss around the implant. This can be confirmed through radiographic assessments.
Diagnostic Tools and Techniques for Identifying Peri-Implantitis:
Accurate diagnosis of peri-implantitis is crucial for developing an appropriate treatment plan. Dental professionals utilize various tools and techniques to identify the condition, including:
Clinical Examination: Thorough visual and tactile assessments are performed to evaluate the gum tissue, probing depths, bleeding on searching, and the presence of suppuration.
Radiographic Evaluation: X-rays and other imaging techniques help determine the extent of bone loss around the implant. This allows for a comprehensive assessment of the condition.
Microbiological Analysis: Collecting samples from the affected site and analyzing the bacteria present can provide valuable insights into the specific pathogens contributing to the infection.
Peri-Implant Probing: Specialized probes measure the pocket depth around dental implants. Increased pocket depth, bleeding, and signs of inflammation indicate peri-implantitis.
Treatment and Management of Peri-Implantitis
When treating peri-implantitis, various approaches can be employed depending on the severity of the condition. Here are some commonly used treatment options:
Non-Surgical Methods: Non-surgical treatments are typically the first line of defense against peri-implantitis. These may include scaling and root planning, meticulous cleaning of the implant surface, and removing bacterial biofilm and calculus deposits. Patients are also educated about proper oral hygiene practices and encouraged to maintain regular dental visits for monitoring and maintenance.
Surgical Intervention: In cases where non-surgical methods are insufficient, or the condition has progressed, surgical intervention may be necessary. Surgical procedures such as flap surgery, bone grafting, guided tissue regeneration, and implant surface decontamination aim to remove infected tissues, restore bone support, and promote healing.
Laser-Assisted Procedures: Laser therapy has shown promising results in managing peri-implantitis. Utilizing specific wavelengths, lasers can selectively remove infected tissues, disinfect the implant surface, and promote tissue regeneration. Laser-assisted procedures offer reduced discomfort, improved healing, and minimal damage to healthy tissues.
The Role of Antibiotics in Peri-Implantitis Treatment:
Antibiotics play a significant role in treating peri-implantitis, particularly in cases where the infection is severe or widespread. They can help control the bacterial infection and prevent further damage. However, a dental professional should always prescribe antibiotic therapy, considering the specific bacteria involved and the patient’s overall health.
It is important to note that antibiotics alone may not be sufficient to treat peri-implantitis. They are often used with other treatment modalities, such as non-surgical or surgical interventions, to achieve comprehensive management.
Laser-Assisted Procedures for Managing Peri-Implantitis:
As mentioned earlier, laser-assisted procedures have gained popularity in managing peri-implantitis. Laser therapy offers several advantages, including:
Precision: Laser technology allows for precise targeting of infected tissues, selectively removing diseased areas while preserving healthy tissues.
Disinfection: Laser heat can effectively disinfect the implant surface and surrounding tissues, reducing the bacterial load.
Improved Healing: Laser therapy promotes enhanced tissue healing and regeneration, facilitating healthy gum attachment and bone support restoration.
One of the Leading Lasers in the Dental Industry is Biolase Epic X Laser. Preferred by Many Dental Professionals in Nationwide.
Proper Management to Prevent Complications:
Proper management of peri-implantitis is crucial to prevent complications and ensure the long-term success of dental implants. Untreated peri-implantitis can lead to further bone loss, implant instability, and implant failure. Therefore, regular monitoring and maintenance visits with your dental professional are essential.
Maintaining excellent oral hygiene practices, adhering to post-treatment instructions, and attending routine dental check-ups are vital to preventing the recurrence of peri-implantitis. By staying proactive and promptly addressing any signs of infection or inflammation, you can preserve the health and longevity of your dental implants.
Prevention and Maintenance
Strategies for Preventing Peri-Implantitis:
Preventing peri-implantitis starts with a proactive approach to oral health. Here are some key strategies to consider:
Excellent Oral Hygiene: Maintaining proper oral hygiene practices is paramount in preventing peri-implantitis. Brush your teeth at least twice daily using a soft bristle and fluoride toothpaste. Remember to floss daily and use an antimicrobial mouthwash to reduce bacterial load.
Regular Dental Check-ups: Routine visits to your dental professional are essential for the early detection of any signs of peri-implant diseases. Regular check-ups allow for timely intervention and preventive measures to preserve the health of your dental implants.
Patient Education: Educating patients about the importance of maintaining good oral hygiene and recognizing the signs of peri-implant diseases empowers them to take proactive measures. Provide comprehensive information about post-implant care instructions and encourage adherence to recommended practices.
Importance of Regular Oral Hygiene and Professional Cleanings:
Regular oral hygiene practices, complemented by professional cleanings, play a significant role in preventing peri-implantitis. Here’s why they are crucial:
Plaque and Biofilm Removal: Professional cleanings remove plaque and bacterial biofilm, which can accumulate around dental implants. This helps prevent inflammation and infection that can lead to peri-implantitis.
Hard-to-Reach Areas: Even with diligent oral hygiene, certain areas around dental implants can be challenging to clean thoroughly. Professional cleanings ensure that these hard-to-reach areas are adequately addressed, reducing the risk of peri-implant complications.
Understanding the Peri-Implantation Window:
The peri-implantation window refers to a critical period after implant placement when the implant is vulnerable to infection and other complications. During this time, proper care and preventive measures are essential. Here’s what you need to know:
Early Intervention: Recognizing and addressing signs of infection or inflammation during the peri-implantation window is crucial. This includes promptly managing conditions such as peri-implant mucositis to prevent progression to peri-implantitis.
Professional Monitoring: Regular follow-up appointments with your dental professional during the peri-implantation window allow for close monitoring of implant healing and early detection of any issues that may arise.
Adherence to Post-Implant Care Instructions: Following post-implant care instructions diligently is essential during the peri-implantation window. This includes avoiding certain foods, practicing oral hygiene, and attending scheduled check-ups.
Controversies and Research
Reversibility of Peri-Implantitis:
Whether peri-implantitis is reversible has been the subject of much debate and investigation. While early intervention and appropriate treatment can effectively manage the condition, it is essential to note that reversing the effects of peri-implantitis entirely may not always be possible.
Several factors contribute to the challenge of complete reversibility, including the extent of bone loss, inflammation level, and underlying systemic conditions. However, with diligent treatment, regular maintenance, and patient compliance with oral hygiene practices, the progression of peri-implantitis can be halted, and the stability and health of the implant can be maintained.
Impact of Excess Cement on Peri-Implantitis:
Excess cement around dental implants has emerged as a potential risk factor for peri-implantitis. When the residual adhesive is left in the peri-implant space, it can create a niche for bacterial colonization and subsequent inflammation. Additionally, the cement itself can induce an immune response, further contributing to the development of peri-implantitis.
Therefore, meticulous removal of excess cement during the placement of dental restorations is crucial in preventing this complication. Dental professionals should adopt appropriate cementation techniques and ensure thorough cleaning to minimize the risk of peri-implantitis associated with excess cement.
The Role of Bacteria in Peri-Implantitis:
Bacterial colonization is a significant factor in the development and progression of peri-implantitis. Just as bacteria play a role in periodontal diseases, they can cause inflammation and bone loss around dental implants. Various bacterial species, including periodontal pathogens, have been associated with peri-implantitis.
Understanding the specific bacteria involved in each case of peri-implantitis is crucial for targeted treatment. Microbiological analysis can help identify the microbial composition and guide appropriate antimicrobial therapy. Moreover, effective oral hygiene practices and regular professional cleanings can help reduce the bacterial load and minimize the risk of peri-implantitis.
Ongoing Research and Advancements:
The field of peri-implantitis is continuously evolving, with ongoing research to improve treatment outcomes and prevention strategies. Advancements in biomaterials, surgical techniques, and antimicrobial therapies offer promising possibilities for managing peri-implantitis effectively.
Staying informed about the latest research findings and advancements is essential for dental professionals and patients. By keeping up with emerging knowledge, we can ensure that our approach to peri-implantitis aligns with the most current evidence-based practices.
CIST Protocol for Peri-Implantitis
Overview of the CIST Protocol:
The CIST protocol is a comprehensive treatment approach that addresses the various aspects of peri-implantitis management. Here’s a breakdown of each component:
Cleaning: Thorough cleaning of the implant surface is crucial to remove bacterial biofilm and calculus deposits. This can be achieved through scaling and root planning techniques specifically designed for dental implants.
Infection control: Effective control of the infection is a crucial aspect of the CIST protocol. This may involve using antimicrobial agents, such as locally delivered antibiotics or antiseptics, to target the specific pathogens contributing to peri-implantitis.
Surgical treatment: In more advanced cases of peri-implantitis, surgical intervention may be necessary. The CIST protocol’s surgical component can include flap surgery, bone grafting, guided tissue regeneration, and implant surface decontamination. These aim to remove infected tissues, restore bone support, and promote tissue regeneration.
Tissue support: Providing support to the regenerated tissues is essential for long-term success. This may involve techniques such as connective tissue grafts or other procedures to enhance the stability and health of the soft tissues around the implant.
Effectiveness and Benefits of the CIST Approach:
The CIST protocol offers several advantages in the management of peri-implantitis. Here are some of its effectiveness and benefits:
Comprehensive approach: By addressing the cleaning, infection control, surgical treatment, and tissue support aspects, the CIST protocol provides a complete solution for managing peri-implantitis. This ensures that all facets of the condition are adequately addressed, leading to improved treatment outcomes.
Targeted treatment: The CIST approach allows tailored treatment based on the patient’s needs. By identifying the specific bacteria involved and customizing the treatment plan accordingly, the protocol maximizes the effectiveness of therapy.
Preservation of dental implants: By effectively managing peri-implantitis, the CIST protocol aims to preserve the health and functionality of dental implants. This helps patients avoid the potential complications and costs associated with implant failure and the need for implant removal.
Long-term success: The CIST protocol focuses not only on immediate treatment but also on long-term success. By promoting tissue regeneration, maintaining infection control, and providing ongoing support, the protocol aims to ensure the longevity and stability of dental implants.
Peri-Implant Fracture and Other Complications
Understanding Peri-Implant Fractures and Their Classifications:
Peri-implant fractures refer to the breakage of the implant or its supporting components. These fractures can occur due to various factors, including excessive forces, inadequate bone support, trauma, or material-related issues. Let’s take a closer look at the classifications of peri-implant fractures:
Biological Classification: This classification system categorizes peri-implant fractures based on the location of the fracture line. It includes the crystal bone, the implant body, or the abutment screw. Each type of fracture has specific implications for treatment and management.
Prosthetic Classification: This classification system focuses on the components affected by the fracture. It includes fractures of the crown, the abutment, or the implant itself. Different prosthetic parts require specific approaches to repair or replacement.
Addressing Other Complications Associated with Peri-Implantitis:
Peri-implantitis can lead to several complications beyond fractures. It is essential to address these complications promptly to ensure the long-term success of dental implants. Here are some common complications associated with peri-implantitis:
Soft Tissue Complications: Peri-implantitis can result in mild tissue complications such as gum recession, increased pocket depth, and inflammation. These issues can compromise the aesthetics and stability of the implant and require intervention to preserve tissue health.
Bone Loss: Progressive bone loss is a significant complication of peri-implantitis. It can compromise the implant’s stability and may require additional procedures such as bone grafting or guided tissue regeneration to restore support.
Implant Mobility and Instability: In advanced stages of peri-implantitis, the implant may become mobile or unstable. This can result from extensive bone loss or damage to the supporting structures. Immediate treatment is necessary to prevent implant failure.
Esthetic Concerns: Complications associated with peri-implantitis, such as gum recession or poor tissue support, can impact the aesthetics of the implant restoration. Addressing these concerns may require procedures such as connective tissue grafting or prosthetic modifications.
Conclusion
Importance of Early Detection and Timely Treatment of Peri-Implantitis:
Early detection of peri-implantitis is crucial for successful treatment outcomes and for preserving dental implants’ health and longevity. By recognizing the signs and symptoms, such as bleeding, inflammation, increased pocket depths, and suppuration, patients and dental professionals can take prompt action to prevent further complications.
Timely treatment interventions, including non-surgical and surgical approaches, laser-assisted procedures, and the CIST protocol, offer effective management strategies. These techniques focus on cleaning, infection control, surgical treatment, tissue support, and addressing potential complications associated with peri-implantitis.
Summary of Key Points Discussed in the Blog:
This blog has explored various aspects of peri-implantitis, including its definition, prevalence, and differentiation from periodontitis and peri-implant mucositis. We have discussed the symptoms and diagnosis of peri-implantitis, highlighting the importance of recognizing early signs and utilizing diagnostic tools and techniques.
We have explored treatment and management options for peri-implantitis, including non-surgical and surgical interventions, the role of antibiotics, and the effectiveness of laser-assisted procedures. We have also emphasized the significance of prevention and maintenance, focusing on strategies for preventing peri-implantitis, the importance of regular oral hygiene, and understanding the peri-implantation window.
Furthermore, we have touched upon controversies and ongoing research in peri-implantitis, discussing the reversibility of the condition, the impact of excess cement, and the role of bacteria. Lastly, we have explored complications associated with peri-implantitis, such as peri-implant fractures and soft tissue and bone-related issues.
In conclusion, early detection and timely treatment of peri-implantitis are vital for preserving the health and functionality of dental implants. By staying proactive, maintaining excellent oral hygiene, attending regular dental check-ups, and promptly addressing any signs of infection or inflammation, patients can ensure the long-term success of their dental implants.


Leave a comment